Isolated Aural Erythromelalgia or Red Ear Syndrome
AUTHORS:
Anusha Tuli1; Ruchita Kachru, MD2; Donna Parker, MD2; Florentina Litra, MD3
1Barnard College, Columbia University, New York, New York
2Department of Pediatrics, University of Florida, Gainesville, Florida
3Department of Pediatrics, University of Florida, Pensacola, Florida
STUDENT ARTICLE | PUBLISHED SPRING 2022 | Volume 42, Issue 2
DOWNLOAD PDF
Case Presentation
An 18-year-old Indian female presented with a one-year history of intermittent redness, burning, and warmth of her ears. The episodes occurred approximately once or twice a day and lasted for about an hour. Only one ear was affected each time but either ear was affected randomly. The episodes did not have any inciting or relieving events, resolved spontaneously, and occurred at any time of the day. There were no associated headaches or migraine episodes, and only the ears were involved without involvement of hands or feet.
Past medical history was significant for attention deficit and her medications included atomoxetine 60 mg daily and oral birth control pills for irregular menses. Review of symptoms was negative for neurological or cardiac symptoms.
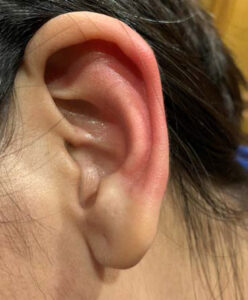
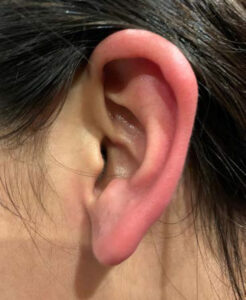
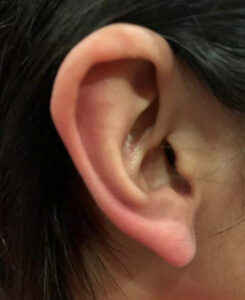
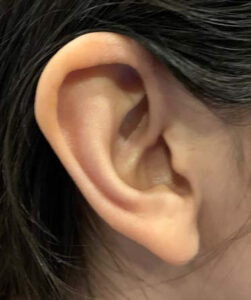
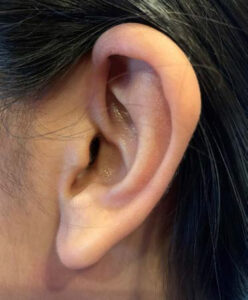
On examination, the patient was an alert and oriented, well-nourished female in no acute distress. Neurological examination was intact. Head and neck examination were normal other than patchy erythema of the right ear with mild edema and increased temperature in the area of erythema. The erythematous area was well demarcated with sharp borders (Figure 1). The other ear was completely normal with no erythema (Figure 2). During the visit, the erythema progressed to involve the entire ear (Figure 3) and then abruptly cleared up (Figure 4). There was no abnormality of the temporomandibular joint and no other autonomic abnormalities. Cardiac examination was within normal limits. Patient was diagnosed with Red Ear Syndrome (RES) and provided reassurance that symptoms would get less frequent in the future. The patient presented subsequently with another episode involving the left ear in a similar fashion (Figure 5).
Discussion
RES is an uncommon disorder typically affecting children and young adults, characterized by intermittent, recurrent episodes of redness, burning and increased temperature of one ear associated with headaches or migraines. It was first described in 1994 and has a slight female preponderance. The episodes can migrate from the ear to the jaw, neck, and even to the occiput.1 The attacks are typically unilateral but may occur on either side, Bilateral attacks and attacks that extend to the face have also been described.2 The cause is unknown, but one theory is that it is a form of trigeminal autonomic disorder resulting in vasodilation.
There are two types of RES. Primary RES is common in those who have migraines as children, teens, and young adults. Secondary RES affects older individuals, especially women, and is commonly seen with temporomandibular joint dysfunction (TMJD), upper spine problems, and headaches.
Common triggers that bring on a case of RES include touching or rubbing of the ear, heat or cold, stress, neck movements, exercise, hair brushing, showering, chewing, or grinding teeth.3 Both types of red ear syndrome have been associated with various conditions, including upper cervical pathology (arachnoiditis, facet joint spondylosis and cervical root traction), glossopharyngeal and trigeminal neuralgia, TMJD, and thalamic syndrome, primary headache disorders (including migraine), chronic paroxysmal hemicranias and hemicrania continua, and the short-lasting unilateral neuralgiform headache with conjunctival injection.4
Proposed mechanisms are “auriculo-autonomic cephalgia” and “cervico-autonomic reflex,” both of which suggest that irritation of the C3 root or great auricular nerve or great occipital nerve lead to release of vasodilator peptides from afferent nerve terminals.2,5-7 Another suggested mechanism is that inhibition of sympathetic vasoconstriction more than activation of parasympathetic vasodilator fibers by the trigemial autonomic reflex is responsible for erythema as well as pain.8 Others have suggested that RES is part of the spectrum of trigeminal autonomic cephalgia, a term that encompass a variety of short-lasting primary headache syndromes associated with autonomic activation.6,9,10 There also may be a connection between the trigeminal nerve and facial parasympathetic outflow. Additionally, local damage to small nerve fibers and vessels has been considered as a possible explanation.2
Diagnostic criteria for RES have been proposed that require at least 20 attacks of ear pain accompanied by redness lasting up to four hours. They must occur more than once daily and must either be accompanied with a burning sensation or triggering by cutaneous or thermal stimulation.2
Erythromelalgia (EM) is a rare disorder characterized by intermittent episodes of redness, warmth, and intense burning pain, but typically affects the hands and feet. It has been suggested that RES associated involvement of hands and feet may be a form of erythromelalgia. It is a rare condition, with a prevalence of 0.36 to 2 per 100,000 patients and has also been classified into primary and secondary forms.11
Primary EM is caused by mutations in SCN9A. This gene encodes the Nav1.7 type sodium channel receptor, expressed in nociceptive neurons and normally amplifies the nociceptive pain signals. Mutations result in familial or sporadic forms of erythromelalgia through dysregulation of these neurons, with dilation of the small vessels. Primary EM may develop at any age.
Secondary EM is commonly associated with myeloproliferative disorders such as polycythemia vera and essential thrombocythemia. EM precedes the onset of the myeloproliferative disorder by 2.5 years in 85% of the cases.11 It can also rarely occur in association with paraneoplastic disorders, diabetes, autoimmune neuropathies, as well as rheumatological and infectious diseases. Secondary EM is seen mostly in adults over 40 years of age. The distal parts of the lower and upper extremities are most commonly involved (hands, feet, fingers and toes). Rarely, symptoms may occur in the face, ears and other parts of the body. The classic description is painful, red, warm hands and feet triggered by warming and downward limb position and relieved by cooling and elevation. The attacks may last minutes to days and typically occur late in the day or night. The quality of life can be greatly affected.
Diagnosis of EM is made based on the triad of recurrent erythema, burning pain and warmth of the affected body part. Family history of EM may support genetic testing, as family planning may be impacted given 50% probability of inheriting the gene mutation in offsprings. A complete blood count should be obtained to screen for myeloprolipherative disorders.
Treatment: While spontaneous remission of symptoms may occur, most cases of RES or EM are refractory to pharmacotherapy. Therapies proposed like cooling, topical capsaicin or anesthetics, medications, or surgical sympathectomy or greater auricular nerve block have had variable responses. The various medications that have been tried include non-steroidal anti-inflammatory drugs, sodium channel blockers, calcium channel blockers, beta blockers, prostaglandins, gabapentin, tricyclic antidepressants such as amitriptyline and imipramine, and methysergide.4
Conclusion
RES is an uncommon disorder typically seen in children and young adults that is usually benign. It may be associated with erythromelalgia, or the two conditions may represent a spectrum with different preferential locations. They are both characterized by dysregulation of the autonomic nervous system and nociceptive neurons by various mechanisms. These conditions do resolve spontaneously without intervention, however therapeutic modalities may be indicated if the condition interferes with daily activities or are very bothersome to the patient. Lifestyle modifications and avoidance of migraine triggers may be useful. Referrals to otolaryngology and neurology may be warranted to rule out secondary causes of RES or EM. Genetic testing may be considered in familial cases and sporadic cases of RES with EM in young adults should trigger a workup for myeloproliferative disorders. However, in most cases, reassurance is all that is needed as it is most often a benign condition.
References
- Lambru G, Miller S, Matharu MS. The red ear syndrome. J Headache Pain. 2013;14:83.
- Brackenrich J SS, Johnston C. Red Ear Syndrome: A Case Presentation and Discussion. HCA Healthcare Journal of Medicine. 2020;1(3):155-159.
- de Amorim IL, Kauppila LA, Martins IP. Red Ear: Syndrome or Symptom? Headache. 2018;58(6):885-891.
- Chan CC, Ghosh S. Red ear syndrome precipitated by a dietary trigger: a case report. J Med Case Rep. 2014;8:338.
- Lance JW. The red ear syndrome. Neurology. 1996;47(3):617-620.
- Goadsby PJ, Lipton RB. A review of paroxysmal hemicranias, SUNCT syndrome and other short-lasting headaches with autonomic feature, including new cases. Brain. 1997;120 ( Pt 1):193-209.
- Moitri MO, Banglawala SM, Archibald J. Red ear syndrome: literature review and a pediatric case report. Int J Pediatr Otorhinolaryngol. 2015;79(3):281-285.
- Fox RH, Goldsmith R, Kidd DJ. Cutaneous vasomotor control in the human head, neck and upper chest. J Physiol. 1962;161(2):298-312.
- Boulton P, Purdy RA, Bosch EP, Dodick DW. Primary and secondary red ear syndrome: implications for treatment. Cephalalgia. 2007;27(2):107-110.
- Donnet A, Valade D. The red ear syndrome. J Neurol Neurosurg Psychiatry. 2004;75(7):1077.
- N. Erythromelalgia. DermNet NZ. 2005.